(01291) 627 374

Chepstow Osteopaths - Back Pain
- Low Back Pain
- Acute or short-term low back pain
- Chronic or long-term back pain
- About The Back
- Causes of low back pain
- Sciatica
- Spinal degeneration - Osteoarthritis and Spinal Stenosis
- Osteoporosis
- Scoliosis Kyphosis and Lordosis
- Spondylosis
- X-ray & MRI
- Exercise
- Medication
- Osteopathic Treatment
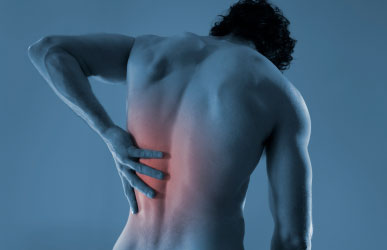
In the UK a third of the population are suffering with back pain and up to 80% of the adult population will suffer significant back pain at some time in their life.
Back pain may be referred to the hip, groin, buttocks, the leg and foot as sciatica.
The main causes of most low back pain are muscular weakness and postural strain due to being overweight, sitting too much, lack of exercise, unequal leg-length, trauma or over-exercise.
Sometimes it is the cushion between the bones (intervertebral disc) which bulges (herniates) and compresses spinal nerves.
As Osteopaths we are specialised in diagnosis of all forms of low back pain and sciatica, using our thorough spinal and clinical examination.
Testing your joints, ligaments, tendons and muscles and using neurological tests of your reflexes, sensation and muscular strength all helps to make an accurate diagnosis of your specific problem.
We treat back pain and sciatica using specific joint manipulation or mobilisation, soft tissue and massage techniques, together with exercise and nutritional advice.
Acute or short-term low back pain
Most acute back pain is mechanical in nature - the result of trauma to the lower back.
Pain from trauma may be caused by a sports injury, work around the house or garden, a sudden jolt from a car accident / whiplash or repetitive stress to spinal joints and musculature.
Symptoms may range from muscle aches to shooting or stabbing pain, Spinal stiffness or an inability to stand upright.
Click here for more information on Whiplash
Chronic or long-term back pain
Chronic back pain is one that persists for more than 3 months.
It is important to diagnose and treat chronic problems sooner rather than later to avoid further gradual degeneration of spinal joints.
Its cause is usually similar to acute back pain however the presence of osteoarthritis / degenerative conditions and postural / occupational factors may have in important role to play here.
The back is an intricate structure of bones, joints, muscles and other tissues that form the posterior part of the body's trunk, from the neck to the pelvis.
The centrepiece is the spinal column, which not only supports the upper body's weight but houses and protects the spinal cord - the delicate nervous system structure that carries signals which control the body's movements and convey its sensations.
Small nerves enter and exit from the spinal cord through spaces between the vertebrae.
The spaces between the vertebrae are maintained by round, spongy pads of cartilage called intervertebral discs, these allow flexibility of the back and act like shock absorbers throughout the spinal column to cushion the bones as the body moves.
Strong ligaments and tendons hold the vertebrae in place and attach the muscles to the spinal column.
As people age their bone strength, muscle elasticity and tone tend to decrease. The discs lose fluid and flexibility which decreases their ability to cushion the vertebrae.
Pain can occur when you lift something too heavy or overstretch, causing a joint sprain or a spasm in one of the muscle groups in the back. A disc may rupture or bulge outward; this can put pressure on spinal nerves. When these nerve roots become compressed or irritated, back pain and ‘sciatica’ often results.
Low back pain may result from nerve or muscle irritation, joint sprain or bone lesions. Most low back pain follows injury or trauma to the back, but pain may be associated with other factors such as degenerative conditions – arthritis, bone or disc disease, osteoporosis or congenital abnormalities of the spine.
Obesity, lack of exercise, pregnancy, stress, poor physical condition, poor posture and poor sleeping position also may contribute to back pain.
Additionally, scar tissue created when an injured back heals itself does not have the strength or flexibility of normal tissue.
A build-up of scar tissue from repeated injuries eventually weakens the back and can lead to loss of normal flexibility and function.
Occasionally, low back pain may indicate a more serious medical problem. Pain accompanied by fever or loss of bowel or bladder control, pain when coughing and progressive weakness in the legs may indicate a severely compressed nerve or other serious condition.
If you are suffering from any of the above please contact your GP urgently.
Sciatica is a condition in which a herniated or ruptured disc presses on the sciatic nerve, the large nerve that extends down from the lower back to its exit point in the pelvis and carries nerve fibres to the leg.
Sciatic nerve compression causes shock-like or burning low back pain combined with pain through the buttocks and down one leg to below the knee, occasionally reaching the foot.
In the more severe cases, the symptoms involve not only pain but numbness and tingling with occasional loss of muscular control in the leg.
click here for more information on sciatica
Spinal degeneration - Osteoarthritis and Spinal Stenosis
Disc wear and tear can lead to a narrowing of the spinal canal especially if the spine has become twisted (scoliosis)
A person with spinal degeneration may experience stiffness in the back on waking and leg pain (sciatica) during walking or while standing for a long time.
Specific and careful Osteopathic treatment may help alleviate postural stress due to degenerative change and help alleviate symptoms.
Osteoporosis is a metabolic bone disease marked by progressive decrease in bone density and strength. Women are four times more likely than men to develop osteoporosis – especially after the menopause. Fracture of brittle bones in the spine and hips results when this condition is allowed to advance untreated.
Scoliosis Kyphosis and Lordosis
Skeletal irregularities and abnormal posture produce strain on the supporting structures of the spine. These irregularities include Scoliosis, a curve or series of curves of the spine to the side; Kyphosis, in which the normal curve of the upper back is severely rounded; Lordosis, an abnormally accentuated forward sway in the lower back or neck.
Gentle Osteopathic treatment together with regular exercises can often help to straighten and mobilise curvatures and minimise spinal pain and stiffness.
Spondylosis refers to chronic spinal degeneration and stiffness, whilst Spondylitis describes inflammation of the spinal joints.
Another painful inflammatory condition of the lower back is Sacroiliitis (inflammation in the pelvic joints).
Spinal X-rays may help diagnose the cause and location of back pain and screen for more serious pathology.
MRI (magnetic resonance imaging) is more useful in evaluating the spine for boney degeneration, disc damage and nerve entrapment as it visualises soft tissue as well as bone.
At the right point in your recovery, exercise is the best way to help yourself strengthen your low back by rebuilding lost muscle tone and strength.
Maintaining and building spinal and abdominal muscle strength is particularly important for people recovering from a spinal injury.
We can provide a list of gentle exercises which help keep muscles moving and speed the recovery process.
A routine of back-healthy activities may include stretching exercises, swimming, walking, and cycling to improve coordination and develop better posture and muscle balance.
Pilates and Yoga are excellent means to gently stretch and strengthen muscles and ease pain.
Medication is often used to treat acute and chronic low back pain.
Anti Inflammatory medication is most effective in the acute phase of most musculo-skeletal conditions but long term use is not recommended.
Spinal manipulation is an effective, proven and safe "hands-on" approach in which a professionally registered practitioner will use specific spinal manipulation together with soft tissue and other complimentary techniques, to improve spinal structure and function.
....would you like some more information or book an appointment?
Use our contact form or call us on the number below:
CLICK HERE to use our form or CALL THIS NUMBER: (01291) 627 374
